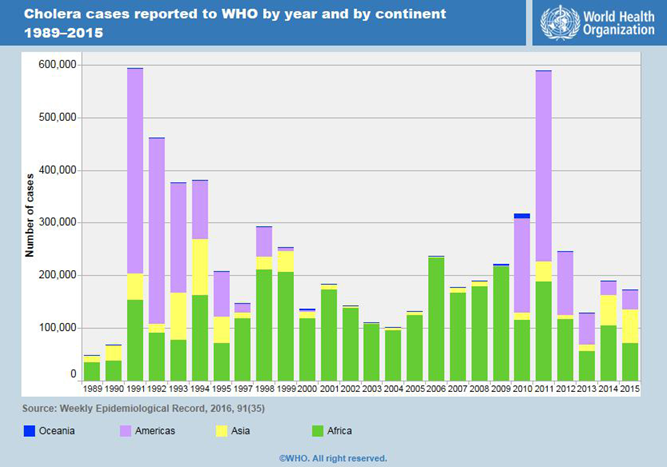
Today, the thought of cholera rarely strikes fear in the hearts of those fortunate enough to be living in developed areas of the world. But in countries where clean water is a privilege and healthcare infrastructure is taxed to its meager limits, cholera is a terrifying prospect. Following the cholera pandemics of the mid-1800s, the disease disappeared from most parts of the world, except Asia, until resurgence in the mid-1970s created the 7th pandemic, which is still continuing in many parts of the developing world (Blake 293). As a result, this ancient disease now joins the ranks as a major global public health threat affecting more than 663 million people living in areas without improved sources of drinking water (WHO 2015).
Within the last two decades both number of cholera outbreaks and number of individuals contracting the disease have been on the rise. Outbreaks in Zimbabwe, Haiti, Senegal, Guinea-Bissau and Vietnam have been characterized by new strains of the disease that are multi-drug resistant and more viral (Blake 293). The recent crisis in Yemen has health officials worried as cases of cholera are doubling within weeks, and the epidemic threatens to “spiral out of control” according Doctors Without Borders.
Implications for emergence of new strains and the threat of bioterrorism are of grave concern to global health experts and scientists alike. Those connections have sparked a renewed interest in the link between infectious diseases and climate. A provocative new article by Erin Lipp, Anwar Huq and Rita Colwell highlights how multi-disciplinary research is being done to create predictive outbreak models for cholera and other diseases (757).
Where cholera is endemic, cases tend to demonstrate distinct seasonal trends. These patterns are strongly related to the ecology of V. cholerae in the environment, where high numbers are observed during times of warm water temperatures and zooplankton blooms (Lipp, Huq & Colwell 759). Antapreet S. Jutla, et. al., explain that “the causative agent of cholera, vibrio cholera, is endemic to brackish riverine, estuarine and coastal waters and is commensal to the copepods (A group of small crustaceans found in the sea and nearly every freshwater habitat, which are sometimes used as biodiversity indicators.) that feed on phytoplankton” (303). Thus, as sea surface temperature rises, phytoplankton increases, which in turn increases the level of the vibrio cholera in the water (Jutla et al 303). Furthermore, Pascual, Mercedes, Menno J. Bouma, and Andrew P. Dobson illustrate that precipitation levels play a large role in vibrio cholera concentrations due to salinity and other factors.
When communities rely on untreated environmental water sources for bathing, cooking and drinking water, incidental ingestion of copepods, which carry a high “dose” of V. cholerae, can initiate an infection. Likewise, likelihood of consuming an infectious dose is higher when a bloom of copepods occurs in the water (Lipp, Huq and Colwell 760). Using climate and other environmental factors to predict where and when cholera outbreaks are most likely to occur can give healthcare workers an advantage in preparing for and limiting the impact of outbreaks.
References:
- Blake, Paul A. “Historical Perspectives on Pandemic Cholera.” Vibrio cholerae and Cholera. American Society of Microbiology, 1994. 293-295.
- Jutla, Antarpreet S. et al. “Warming Oceans, Phytoplankton, and River Discharge: Implications for Cholera Outbreaks.” The American Journal of Tropical Medicine and Hygiene2 (2011): 303–308. PMC. Web. 22 May 2017.
- Lipp, Erin K., Anwar Huq, and Rita R. Colwell. “Effects of Global Climate on Infectious Disease: The Cholera Model.” Clinical Microbiology Reviews4 (2002): 757-770.
- Mendelsohn, Joshua, and Terry Dawson. “Climate and Cholera in KwaZulu-Natal, South Africa: The Role of Environmental Factors and Implications for Epidemic Preparedness.” International Journal of Hygiene and Environmental Health 211.1 (2008): 156-162.
- Pascual, Mercedes, Menno J. Bouma, and Andrew P. Dobson. “Cholera and Climate: Revisiting the Quantitative Evidence.” Microbes and Infection 4.2 (2002): 237-245.
- World Health Organization (WHO), http://www.who.int/gho/epidemic_diseases/cholera/en/